Background:
Primary testicular lymphoma (PTL) accounts for 1% to 2% of non-Hodgkin's lymphomas. Diffuse large B-cell lymphoma (DLBCL) is the most common histological subtype of PTL, accounting for 80% to 98% of cases. The introduction of rituximab was a breakthrough in DLBCL treatment. However, the impact of rituximab on primary testicular DLBCL (PT-DLCBL) is controversial. A study by Gundrum et al (Gundrum JD, et al. J Clin Oncol 2009) found that PT-DLBCL survival did not improve in the rituximab era (i.e., after 2000). However, that study was based on a Surveillance, Epidemiology, and End Results (SEER) database cut-off of 2005. The follow-up period of PT-DLBCL patients in the rituximab era was relatively short, at only 4 years (from 2001 to 2005). Considering the wide use of rituximab in all kinds of DLCBL, we conducted a study based on the SEER database to evaluate the potential impact of the introduction of rituximab on PT-DLBCL.
Methods:
Data from the SEER 13 registries were analyzed in this study. Cases with PT-DLBCL diagnosed from 1992 to 2018 were included. Baseline characteristics, including age at diagnosis, laterality (left, right, bilateral), age, race, Ann Arbor stage, SEER cause-specific death classification, survival months, and vital status, were collected. Cancer-specific survival (CSS) was used as the study endpoint and defined as the time from diagnosis to death from DLBCL or last follow-up. The Kaplan-Meier method was used to build survival curves and the log-rank test used to compare groups. All p values were two-sided, and p-values < .05 considered statistically significant. All analyses were conducted using GraphPad PRISM 6.
Results:
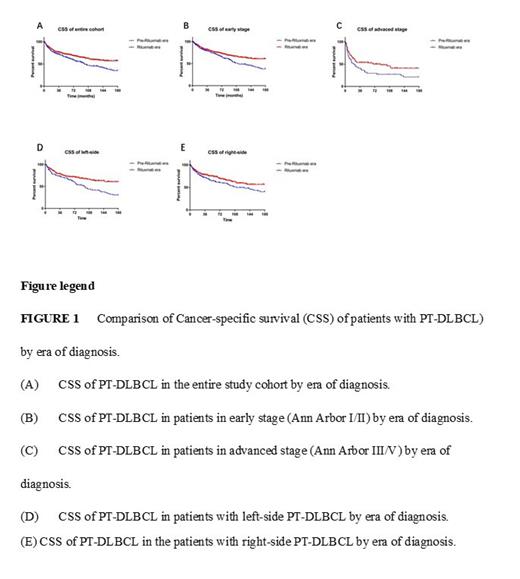
A total of 961 patients were included in this analysis. Among them, 271 were diagnosed from 1992 through 2000 (pre-rituximab era) and 690 from 2001 through 2018 (rituximab era). In all, 435 patients showed unilateral left-side testicular involvement, 455 right-side, 63 bilateral, and 8 unknown. At last follow-up, 489 patients had died of PT-DLBCL. Patients diagnosed in the pre-rituximab era had more stage I disease than their counterparts in the rituximab era. No difference was found in age, race, or laterality across the two eras. For the entire cohort, there was a significant improvement in CSS in the rituximab era compared with the pre-rituximab era. The median CSS in the pre-rituximab era was 98 months compared to not reached in the rituximab era ( p = .001) (Figure 1A). We also compared the CSS of patients in different stages: early stage (I/II) or advanced stage (III/IV) in the pre-rituximab and rituximab eras. We found that CSS improved significantly in either early or advanced stage (early stage, p < .0017; advanced stage, p = .026; Figure 1B and 1C). We also explored the role of laterality in survival of PT-DLBCL. Compared with the pre-rituximab era, CSS of either left-side (Figure 1D) or right-side (Figure 1E) PT-DLBCL improved significantly (left-side, p < .001; right-side, p = .04) in the rituximab era. The introduction of rituximab decreased CSS by about 50% in patients with left-side PT-DLBCL but only about 30% in those with right-side disease, which indicated that patients with left-side (vs right-side) PT-DLBCL derived greater survival benefit from the introduction of rituximab.
Conclusions:
Survival of PT-DLBCL patients improved significantly in the rituximab era, with the survival curve reaching a plateau from the tenth year after treatment. Patients with left-side (vs right-side) PT-DLBCL derived greater survival benefit from the introduction of rituximab.
Disclosures
No relevant conflicts of interest to declare.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal